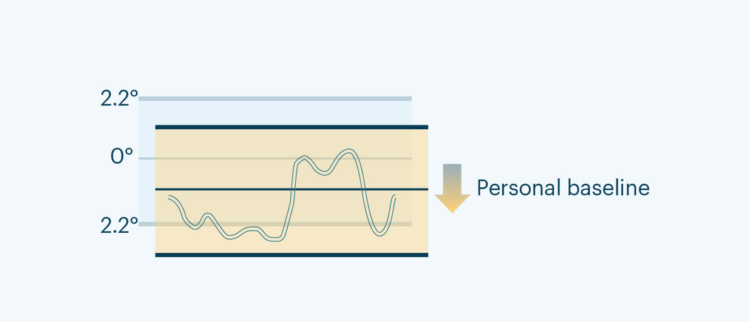
Diabetic Foot Ulcer Stages and Classification Systems
It is important to ensure that a medical provider is utilizing the most accurate, reliable, and up-to-date classification system when diagnosing and treating a diabetic foot ulcer. There are 37 total classification systems, of which 19 have been determined to be reputable after strict critical review.1
In order to be considered as a classification system, people had to be sorted based upon various risk factors which were either present or absent. In addition, a point system detailing the severity of each risk was included, with the lowest number being the least severe and the highest number being the most severe.
Of these reputable classification systems, there are two that are considered to be the most accurate, and as such, are the most widely used among medical practitioners. These are called the University of Texas Diabetic Foot Ulcer System and the Wagner Diabetic Foot Ulcer System (hereafter referred to as the DFU system).
How To Classify Diabetic Foot Ulcer Stages
No two DFU systems are the exact same, and none are universally accepted. On average, many of the systems rate the advancement of diabetic foot ulcer stages by:
- Wound size
- Wound depth
- If the wound is clean or infected
- If the wound is neuropathic, ischemic, or neuroischemic
Some DFU systems utilize all of these factors, and some only use a few. The two most widely used DFU systems are covered in more detail below.
What Is Diabetic Foot?
Diabetic foot is a common, and severely dangerous, complication that occurs in around 15% of people with diabetes.2 The severity of this condition cannot be understated, as when left untreated, diabetic foot ulcers often lead to infection, gangrene, and may require amputation.
This condition can happen in anyone with diabetes but is it more common in people with unmanaged diabetes, or diabetes that has worsened through poor diet, lack of exercise, or inadequate medication.
If caught early, the condition can be treatable, and significant side effects can be avoided. The type of treatment that will be necessary depends entirely on the size and location of the foot ulcer. Using a diabetic foot staging and classification system can help in determining treatment options for patients.
If left untreated, the condition can potentially lead to a lower extremity amputation. Nearly 85% of amputations that are the result of diabetes can be prevented with early treatment. At the same time, 85% of lower extremity amputations are preceded by a foot ulcer that goes untreated.3
Many patients with diabetes have an additional condition known as peripheral neuropathy (PN). PN occurs when nerves are damaged or destroyed which prevents the brain from sending messages throughout the body, including a person’s feet.
For patients with diabetes, this often results in numbness in the feet and a loss of pain sensation, which can make it difficult for them to notice when they have cuts, blisters, or sores on their feet.4
Because of this, it is imperative that people with diabetes check their feet daily to ensure that they have not been injured. If an injury has occured, such as redness, cuts, blisters, or an open wound, they should seek medical advice from their doctor as soon as possible to ensure that they receive proper treatment.
University Of Texas Diabetic Foot Ulcer Stage System
The University of Texas DFU system evaluates three major risk factors when determining the severity of a patient’s diabetic foot ulcer. These factors are wound depth, presence or absence of infection, and presence or absence of ischemia (a reduction in blood flow).
An ulcer’s wound depth is measured in 4 grades going from 0-3, and the presence of ischemia and/or infection is measured in 4 stages from A-D. This method is effective at predicting the likelihood of lower extremity amputation, and it is thought to be more descriptive than many other DFU systems.5
Stages/Grades
| Stage/Grade6 | 0 | 1 | 2 | 3 |
|---|---|---|---|---|
| A | Pre or post ulcerative lesion completely epithelialized | Superficial wound not involving tendon, capsule, or bone | Wound penetrating to tendon or capsule | Wound penetrating to bone or joint |
| B | With infection | With infection | With infection | With infection |
| C | With ischemia | With ischemia | With ischemia | With ischemia |
| D | With infection and ischemia | With infection and ischemia | With infection and ischemia | With infection and ischemia |
The Wagner Diabetic Foot Ulcer Classification System
Occasionally referred to as the Merritt-Wagner system, the Wagner DFU system was invented in the 1970s. Despite its simplicity with regard to grades, it is also considered highly accurate in predicting the outcome of an ulcer and the likelihood of lower extremity amputation.7
The Wagner DFU system is the system that is required to be used for patients who have Medicare as their primary insurance. Certain treatments, such as hyperbaric oxygen therapy, cannot be considered or covered for a patient unless they are staged as Grade 3 or higher and have not had results with conventional treatment over a period of 30 days.8
Grade 0: Intact skin
Grade 1: Superficial ulcer
Grade 2: Intact skin
Grade 3: Ulcer with bone involvement
Grade 4: Forefoot gangrene
Grade 5: Full-foot gangrene
What Is A Wagner Grade 1 Ulcer?
A Grade 1 Ulcer on the Wagner DFU system is considered a superficial ulcer with partial or full-thickness. These wounds may have penetrated the epidermis and dermis, however, they have not reached the tendon or bone yet.
Essentially, this is the farthest stage that a patient would ideally be diagnosed at as the possibility for treatment, and the likelihood of recovery is significantly increased because the wound has not fully penetrated the foot yet.
How Diabetic Foot Ulcers Start
Most diabetic foot ulcers occur most commonly on the balls of the feet, under the big toe, or on the metatarsals, which are the balls of the feet.9 They can occur for several reasons including:
- Injury
- Obesity
- Poor hygiene
- Heart disease
- Hyperglycemia
- Kidney disease
- Poor circulation
- Poorly fitting shoes
- Sustained Pressure
- Tobacco or alcohol use
- Causing trauma to the skin when cutting toenails
While these are some of the most common causes of diabetic foot ulcers, this is by no means an exhaustive list.
What The Start Of A Foot Ulcer Looks Like
It can be difficult for a person with diabetes to realize that they have a diabetic foot ulcer until it has already progressed. The reason for this is that many people with diabetes do not have feeling in their extremities due to poor circulation and peripheral neuropathy, so they may not feel the pain of a cut or wound.
One of the first signs of a diabetic foot ulcer that a person with diabetes may notice is drainage from the wound that stains their socks. Irritation, swelling, or an unpleasant odor may also be some of the first signs that a diabetic foot ulcer is present.
In more severe cases, a person may notice discoloration around the wound (which may be black in color), or the skin around the wound may be callused or painful to the touch.
If these symptoms are present, immediately seek medical care, ideally with a podiatrist, to prevent the wound from getting any worse and begin treatment as needed.
What Happens When A Person With Diabetes Gets A Cut On Their Foot
People with diabetes do not heal as quickly as people without diabetes. Because of this, what may be a minor cut that doesn’t require anything more than a quick cleaning for most people can be deadly for a person with diabetes.
The following information is guidance only. Please consult with a medical professional if you are concerned about your foot health.
When a person with diabetes gets a cut on their foot, they should thoroughly clean and bandage the wound immediately, and they should check the wound every day to ensure that it is healing. If the wound is not showing signs of healing after the second day then it is time to contact the doctor to ensure that it does not turn into a diabetic foot ulcer.
If the wound is not healing then the patient begins to risk developing an infection. Infections are significantly more difficult to treat in patients with diabetes, and they can at times lead to the formation of a diabetic foot ulcer and/or amputation. Some serious signs of infection to look out for include:
- Chills
- Fever
- Drainage or pus
- Swelling or inflammation
- Redness around the wound
- Throbbing in the affected limb
- Unusual heat in the wound area
- Foul smells or unpleasant odors from the wound
It is highly encouraged that a person with diabetes work to prevent a diabetic wound from happening in the first place.
How To Prevent Getting A Diabetic Wound
It is much easier to prevent a diabetic wound from happening than it is to try to treat it.10 The most effective method of preventing a diabetic foot wound is by reducing as many of the patient’s risk factors as possible. These risk factors have been listed above.
In addition, they should also begin diligently checking their feet every day for any potential signs of damage. One should check all areas of the feet including the toes, between the toes, the heels, the sole, and the sides and top of the feet.
Some things to look for include:
- Cuts
- Ulcers
- Cracks
- Calluses
- Blisters
- Bruising
- Irritation
- Redness
- Soreness
A patient should Immediately care for any abnormalities that they discover and they should watch them to ensure that they are healing properly. In addition, it is important for a patient with diabetes to get their feet regularly checked by their doctor during check-ups to ensure that there is nothing that they may have missed.
Additionally, it is important for patients to take good care of their feet. A patient should ensure that they thoroughly wash and dry their feet daily and they should regularly change their socks to prevent them from getting damp. It can also help patients to keep their feet moisturized and to keep their nails trimmed neatly, but not extremely short.
It is essential to wear shoes that properly fit and are high quality whenever the patient goes out. Finally, they should see a podiatrist on a regular basis to make sure that any corns, calluses, or other foot conditions are taken care of properly to reduce the chances of developing a diabetic foot wound.
The American Podiatric Medical Association (APMA) recommends people with diabetes schedule a foot exam with their podiatrist at least once a year to help maintain foot health.11
How Long Does A Foot Ulcer Take To Heal?
The healing time required largely depends on the size and depth of the diabetic foot wound. Other factors may be if the wound is constantly agitated from pressure or being rubbed on by a sock or shoe, lack of proper circulation, sustained high pressure, and other co-existing health conditions.
Under optimal conditions, and with a shallow Grade 0-1 diabetic foot ulcer, healing can occur in as little as 3-6 weeks. More severe ulcers, particularly ones that have penetrated deeply into the muscle or bone, can take as long as 12-20 weeks to properly heal.
It is important to note that these are considered optimal timelines for healing and that they consider that a patient is taking proper care of their wound and following all instructions that have been given to them by their doctor.
Any size diabetic foot ulcer has the potential to become infected and turn gangrenous if left untreated. These wounds are extremely serious and should be treated as such.12
How A Diabetic Wound Can Heal Faster
The best way that a person with diabetes can help their diabetic foot ulcer heal faster is by improving their overall lifestyle and following instructions from the doctor as closely as possible.
During the initial treatment, the patient's doctor will determine their treatment plan based on the severity of their wound. For a wound that still has good circulation, their doctor will likely start the treatment by debriding the wound.
This is a process by which the doctor carefully removes any of the diseased tissue from around the wound to keep the wound from expanding further. Once the debridement is complete, the doctor will apply a dressing bandage that will help keep the wound clean and free of debris.
They will also have to see their doctor on a regular basis to ensure the wound is healing, and additional debridements may be required.
Additionally, their doctor may recommend “off-loading”. Braces, specialized footwear, a boot, crutches, or a wheelchair may be provided to assist the patient in keeping pressure off of the affected area.
Some patients may benefit from the use of the Orpyx SI® Sensory Insole System, which can provide real-time alerts to notify the wearer when there are high foot pressures occurring which can lead to wounds. By measuring the patient’s plantar pressure, temperature, adherence, and step count data, a more comprehensive care plan can be put together to help the patient prevent these foot ulcers from recurring.
Why Your Diabetic Foot Ulcer Healing Is Slowly
There are several factors that can interfere with the healing process of a diabetic foot ulcer. The most significant of these are high blood sugar levels, which can be common in patients with diabetes.
Hyperglycemia can interfere with the way that a patient’s body metabolizes nutrients and absorbs oxygen, and it can cause inflammation as it prevents their immune system from working efficiently.
Many patients with diabetes also have peripheral vascular disease which restricts blood flow to their limbs. This interacts negatively with a higher level of glucose in the blood system and makes circulation less effective.
This all makes it much more difficult for the immune system to perform its job, which is what can cause a diabetic foot ulcer to take so long to heal.13
How To Prevent Complications When Healing
It is important for patients to follow their doctor’s instructions exactly and to keep any follow-up appointments. They should Immediately let their doctor know if they think that there may be something wrong with their wound or if they notice any signs of infection in the affected area.
A patient should ensure that their bandages are kept clean, that they are changed regularly, and that they are taking any medications that their doctor prescribed as directed. Keep pressure off of the wound as often as possible by following the doctor’s prescribed “off-loading” instructions.
Will Diabetic Foot Ulcers Ever Heal?
Roughly 86% of diabetic foot ulcers heal successfully within a year of treatment.14 The time of treatment can vary widely, with some ulcers only taking 3 weeks to heal and others taking as long as a year. After healing, 49% of wounds recurred within the first year after treatment, and there was a 68% recurrence within 5 years.15
With early intervention, treatment is significantly more effective and does not take as long as it will if the wound is allowed to worsen before seeking medical care. In many cases, once an ulcer has been fully healed, it is possible to prevent it from reopening or becoming reinfected through careful observation and preventative foot care.
Not all diabetic foot ulcers properly heal, however. Roughly 12% of these ulcers remain unhealed and progressively worsen to the point where amputation becomes necessary.16
Some Healing Factors For Diabetic Foot Ulcers
We now know more about diabetic foot ulcers than ever before. Through constant research into diabetes and how it affects people, several DFU risk and classification systems have been created that help to serve as an early warning system of how far along a patient’s diabetic foot ulcer may be.
Early diagnosis and proper wound care are essential in giving patients the best chance to heal their diabetic wounds. Once an ulcer has been diagnosed and a treatment plan has been decided upon, it is imperative that the doctor’s orders be followed exactly.
All follow-up appointments should be kept, and the wound dressing should be changed on the schedule that the doctor recommends. Make sure that the patient is “off-loading” their foot when possible to keep pressure and irritation from worsening the wound.
Ensure that the patient or caregiver that is caring for them is performing daily foot checks to gauge the healing process. If the wound looks like it is not healing, the doctor should be immediately informed so that the treatment process can be adjusted.
Additionally, it is important for the patient to maintain a healthy lifestyle. This includes keeping their diabetes under control, watching their diet and weight, exercising as often as possible, and not smoking and drinking. This will give the patient their best chance at healing their diabetic foot ulcer.17
Why A Diabetic Foot Ulcer Is Not Healing
The most common reasons that a diabetic foot ulcer is not healing include:
- Hyperglycemia
- Poor circulation
- Smoking or drinking
- Insufficient or improper wound care
If a patient believes that their diabetic foot ulcer is not properly healing, or if they can’t see any signs of improvement, the patient should inform their doctor. It may be necessary to adjust the treatment method or to try something else entirely to help the wound heal.
What Happens If A Foot Ulcer Doesn't Heal?
In the worst-case scenario, a diabetic foot ulcer that won’t heal can lead to an amputation. The severity of the diabetic foot ulcer, its location, and how far the infection has spread will determine the type of amputation that is necessary. 18
Most commonly, this situation will lead to a lower extremity amputation that typically consists of amputation of the toes, feet, or lower legs. In some cases, however, the infection may require above-the-knee amputation.
Scientists and doctors are constantly studying the effects of diabetes and are learning new ways to help those with diabetes learn to manage and live with their condition. In the past twenty years, the rate of lower limb amputations in those with diabetes has been reduced by 50%. With continuing study and proactive foot care, this rate will hopefully continue to get lower in the future.19
What is Peripheral Neuropathy? - The Foundation For Peripheral Neuropathy (https://www.foundationforpn.or...)
Data on file Diabetic Neuropathic Foot Ulcer Recurrence; October 2020. 2. Apelqvist J, Larsson J, and Agardh C.D. (1993). Long-term prognosis for diabetic patients with foot ulcers. Journal of Internal Medicine 233(6): 485-491.